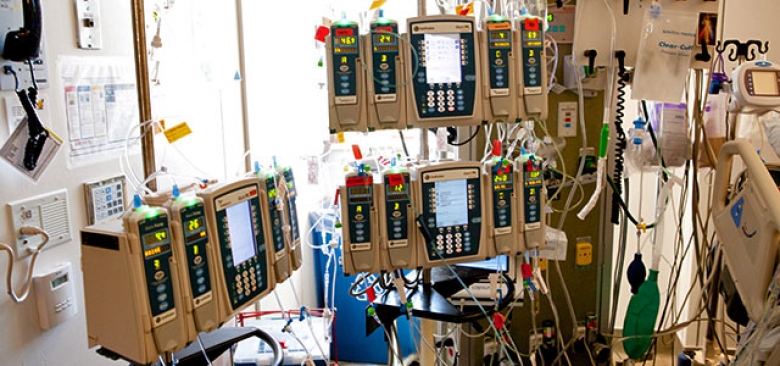
Alarm fatigue is a real problem in hospitals, resulting in serious consequences for patient safety. It occurs when clinicians become desensitized to the sound of alarms due to their overuse. In order to reduce alarm fatigue and ensure a safe environment for patients, it’s important for hospital staff to take certain steps. This article outlines 8 potential ways to reduce alarm fatigue in hospitals and improve patient safety.
The sheer number of alarms within hospital rooms can cause alarm fatigue. The clinician experiences sensory overload from excessive alarm numbers and becomes desensitized resulting in longer response times or critical alerts missed altogether. According to a recent study, alarm alert overload has the highest potential impact on healthcare systems. No matter what the scale of the hospital, you’ll probably hear alarm bells buzzing throughout the day. The modern healthcare system provides an extremely computer-driven clinical environment that makes most everything connected to a monitor which can produce audible noises.
Tell me about the alarm fatigue of nurses.
Alarm fatigue is a serious problem for nurses in hospitals, as they are surrounded by beeping machines and alerts. It can lead to mental exhaustion, decreased job satisfaction, and even medical errors due to increased distraction. To reduce alarm fatigue among nurses, there are several steps that can be taken.
First, hospitals should create an environment where alarms are only used when absolutely necessary. This means limiting the number of alarms that go off at any given time and ensuring that all staff members are aware of which alarms indicate a serious situation requiring immediate attention. Additionally, hospitals should review each patient’s individual alert settings to ensure they make sense based on their condition and the care they need.
Second, hospitals should have strict protocols in place for responding to alarm signals. These protocols should ensure that all staff members understand who is responsible for responding to which alerts and how quickly they must respond when one goes off. Furthermore, hospital leaders should provide training on how best to respond to various alarm signals so that nurses do not become overwhelmed or confused about what action needs to be taken in response.
Rob Wilder, Director of Product Management
Rob Wilder serves as the Director of Product Management at a leading healthcare technology company. He has many years of experience in the healthcare industry and is an expert on issues related to patient safety, medical device management, and alarm fatigue. Rob is passionate about improving the quality of care provided to patients by tackling alarm fatigue through innovative product design.
Rob leads initiatives that focus on streamlining communication between multiple departments within hospitals and ensuring alarms are set appropriately based on each patient’s individual needs. His team works with hospital staff to identify areas where alarms can be optimized or replaced with alternative solutions in order to reduce unnecessary noise and confusion for clinicians.
Another key component of Rob’s efforts is identifying ways that hospitals can better respond when an alarm does sound. To do this, he works closely with staff to create protocols for responding quickly and effectively when an alarm indicates a possible health concern for a patient. Additionally, Rob focuses on developing hospital-wide standards for how alarms should be set up and monitored so everyone involved knows what they need to do when one sounds off.
False, Nonactionable, and Nuisance Alarms
False alarms are generated when the alarm monitoring system produces an alert that is not related to a real physiological or environmental condition. Nonactionable alarms occur when there is no clinical action required in response to the alarm, and nuisance alarms are those that generate frequent false or nonactionable alerts. Reducing false, nonactionable, and nuisance alarms requires three key actions: modifying existing alarm settings, instituting protocols for maintaining optimal sensitivity of monitored parameters, and utilizing technologies to improve the accuracy of patient-monitoring systems.
Modifying existing alarm settings involves adjusting sensitivities so that only relevant data is monitored, which reduces unnecessary noise from the system. Protocols should be implemented regarding how often sensor readings should be rechecked for accuracy and how frequently monitoring systems need to be recalibrated; this reduces false readings from faulty sensors. Finally, new technologies such as artificial intelligence-based algorithms can help filter out irrelevant information from patient monitors and alert staff members only when clinically relevant conditions arise.
Alarm. Fatigue
Alarm fatigue is a real problem in hospitals, and one of the most important ways to reduce it is to make sure alarms are set to the right volume. Ensuring that only relevant critical alarms are enabled can help decrease alarm fatigue. Alarms should be properly customized for each patient so that patients are not receiving alarms that aren’t relevant or necessary for their health. Additionally, staff should be well-trained on when and how often alarms should sound, and which alarm sounds signal certain issues.
This helps ensure that staff knows what they’re hearing and why they’re hearing it. The use of visual indicators as well as audible alarms can also be effective in reducing alarm fatigue by providing an alternative form of notification without relying solely on an auditory alert. Finally, having clear policies regarding the proper response time for responding to an alarm can help decrease unnecessary alarms from going off because staffers feel rushed. Taking these steps can help reduce hospital-wide alarm fatigue and make healthcare safer for everyone involved.
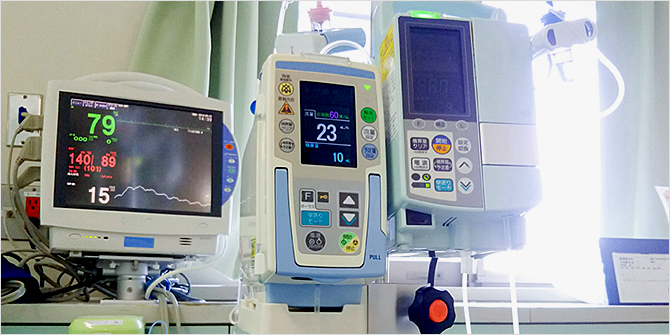
Example alerts from monitoring devices
Alarms from monitoring devices in hospitals can often lead to alarm fatigue among staff when used without proper management. To reduce this issue, healthcare organizations should consider the following strategies:
1. Establish an alarm management committee: This committee should be responsible for establishing and enforcing policies for managing device alerts. They should also set protocols for validating alarms, providing feedback on alert performance, and addressing any issues related to false positives.
2. Implement a proactive approach: Healthcare organizations should proactively assess the accuracy of their device alarms by analyzing data from past experiences with alerts, as well as identifying potential areas of improvement. This approach can help ensure that alarms are both accurate and actionable when they occur.
3. Utilize technology-based solutions: Technology-based solutions such as automated alerting systems can help reduce manual processes associated with setting up alerts and enable more targeted responses to patients’ needs—while also reducing the number of false positives generated by medical devices.
Organizations make changes to avoid dangers
Organizations must stay informed of the dangers of alarm fatigue, and take action to avoid them. One way is to ensure that alarms are set up properly. Alarms should not be too loud or too quiet, but instead at a volume that can easily be heard throughout the hospital. This can help reduce the number of false alarms and make it easier for staff to respond quickly when there is an actual emergency.
Additionally, organizations should invest in reliable alarm systems with consistent monitoring capabilities. This ensures that all alarms are managed properly and responded to in a timely manner. Finally, organizations should develop protocols for responding to each type of alarm so that staff are prepared for any situation they may encounter. By making these changes and taking preventative measures, organizations can reduce the risk posed by alarm fatigue and keep their patients safe from harm.
Read Also…Computer Systems Analysts
What is alarm fatigue?
Alarm fatigue is a term used to describe the phenomenon wherein healthcare professionals become desensitized to frequent alarms due to over-exposure. Common sources of these alarms include medical equipment such as patient monitors, ventilators, and infusion pumps. Continuous exposure to false or unnecessary alarms can cause healthcare practitioners to ignore them altogether, leading to serious consequences for patients. In order to reduce alarm fatigue in hospitals, there are several steps that can be taken.
First, it is important for healthcare personnel to be properly trained on how and when alarm systems should be used, as well as strategies for alerting the right people at the right time. Additionally, hospitals should set standards regarding their use of alarm systems, including which types of alarms should be used in different scenarios and acceptable levels of noise pollution from alarms within a given environment.
Furthermore, healthcare providers should also consider implementing systems that prioritize urgent alerts over non-urgent ones so that staff members are not overwhelmed with an excessive number of low-priority notifications. Finally, it is important for hospitals to invest in high-quality alarm systems with reliable sensors and accurate detection capabilities so that staff members trust the alerts they receive and respond accordingly when needed.
1. Education & Training
Excessive noise levels in hospitals created by medical equipment alarms can lead to a phenomenon known as alarm fatigue. This is when clinicians become desensitized to the sound of alarms, leading them to either ignore or respond too slowly to alerts that could be critical for patient care. To reduce the impact of this problem, healthcare organizations should consider implementing the following strategies:
1. Education & Training: By providing education and training on how to properly use and adjust medical equipment alarms, hospital staff will be better informed on how they can reduce noise pollution while still ensuring timely responses. Additionally, regularly scheduled refresher courses and simulations can help keep staff up-to-date on changes in technology and best practices for alarm management.
2. Alarm Management Policies: Developing guidelines for when and how often an alarm should sound can prevent unnecessary distractions from alerting clinicians about low-priority activities like meal time or scheduling conflicts. Furthermore, setting limits on the types of noises an alarm system produces ensures that only high-priority alerts stand out from background noise levels without being overly jarring or disruptive.
3. Technology Upgrades: Installing new technology such as smart bedside monitors with analytics capabilities not only improves patient safety but also reduces false alarms due to its ability to detect real-time changes in a patient’s condition more accurately than manual systems do. Additionally, incorporating wireless protocols into existing devices also helps minimize unnecessarily loud noises while still allowing clinicians to receive important information quickly and efficiently.
2. Alarm Settings
Alarm settings are a key component of reducing alarm fatigue in hospitals. Alarms should be set at realistic levels to ensure that clinicians have time to respond without being overwhelmed by too many alarms. To achieve this, hospitals and healthcare facilities should strive for a system-wide approach when setting alarms, rather than individual clinicians making their own decisions about what each patient’s alarm settings should be.
Additionally, the thresholds for alarms should be based on evidence-based practices rather than individual preferences or past practices. Lastly, nurses should review alarm settings regularly to make sure they are still appropriate and need not be changed due to changes in a patient’s condition or vital signs. In this way, keeping appropriate alarm settings can help reduce the number of unnecessary alarms that contribute to alarm fatigue in hospitals.
3. Proactive Monitoring
Proactive monitoring seeks to reduce alarm fatigue by proactively identifying and addressing possible system failures before they become critical issues. This can be done through predictive analytics, which uses data from multiple sources such as patient records, vital sign readings, and alarms to detect patterns and identify anomalies that may lead to a potential issue. By detecting problems early, hospitals can address them quickly before they become serious issues.
Additionally, proactive monitoring can help ensure compliance with regulatory requirements such as the Joint Commission’s National Patient Safety Goals. The main goal of proactive monitoring is to provide more efficient care by reducing the number of unnecessary alarms that are generated due to false positives or system errors. Implementing this type of monitoring also helps increase staff satisfaction by decreasing alarm fatigue and ensuring that teams have access to the most up-to-date information about their patients’ conditions in real-time.
4. Standardize Technology
Standardizing technology is key to reducing alarm fatigue in hospitals. Having a standardized system of equipment, alarm settings, and protocols simplifies the processes for both staff and patients. It ensures that everyone knows what alarms mean, what action needs to be taken when an alarm sounds, and who should respond to an alarm. Standardizing also helps reduce the number of false alarms that can overwhelm healthcare workers and lead to alarm fatigue.
Additionally, streamlining different types of medical devices into one central monitoring system ensures that clinicians have access to all patient data at once. This allows them to quickly see changes in vital signs which reduces response times and potential negative outcomes due to delayed reactions or incorrect diagnoses. It also prevents unnecessary notifications from multiple devices which can overload staff with unnecessary information leading to confusion and distraction from important tasks. By standardizing technology, hospitals can prevent these issues while ensuring positive patient outcomes by providing quick responses in case of emergency situations.
5. Assign Responsibility
Once responsibility is assigned, the team should ensure that everyone understands the roles and expectations. The team leader should have a clear plan of action that outlines who will implement each step of the process and how they will go about it. It’s also important to ensure that everyone is held accountable for their role in reducing alarm fatigue.
This can be done through regular communication regarding progress and feedback from team members. Additionally, by assigning specific tasks to each person on the team, it allows for an efficient division of labor and encourages collaboration among members. With a defined set of responsibilities for each individual, it’s easier to monitor successes and failures within the project, ensuring that any problems are addressed quickly before they become harmful to patient care.
6. Reduce False Alarms
One way to reduce false alarms in hospitals is to use alarm management technology. This type of technology can be used to monitor multiple alarms at once and alert staff only when necessary. Alarm management software can also be used to customize alarm settings for each patient, allowing nurses and doctors to set thresholds that are appropriate for each individual’s needs. Additionally, this type of software can provide analytics on the frequency, duration, and severity of alarms so that hospital personnel has a better understanding of how their patients are responding to treatment.
Another way to reduce false alarms in hospitals is by using evidence-based clinical guidelines. These guidelines provide steps that healthcare professionals should follow when dealing with particular medical conditions or treatments. By following these guidelines, medical staff can ensure they are making decisions based on the most up-to-date research and best practices available. Clinical guidelines also help standardize care across multiple departments within a hospital setting; this helps reduce errors caused by inconsistencies in procedures between different units or hospitals.
Finally, healthcare providers can utilize predictive analytics tools such as machine learning algorithms or computer-aided diagnostics (CAD) systems to anticipate situations where alarm fatigue may occur before it does. By providing early warnings about potential problems or adverse events before they actually occur, hospital staff can take steps proactively to prevent false alarms from occurring in the first place.
7. Implement a Policy of Silence
Having a policy of silence encourages hospitals to reduce the amount of noise and distractions, which can lead to alarm fatigue. This policy involves limiting conversations in patient rooms and areas with high-acuity patients, using quiet alarms instead of loud ones when possible, and avoiding unnecessary equipment sounds or beeping noises. Developing workflows that involve fewer frequent alarms is also important; for instance, scheduling rounds at regular intervals instead of having a nurse check on each patient regularly throughout the day will help minimize disruption. Finally, training staff members on how to appropriately respond to alarms — including how to prioritize them — is essential for reducing alarm fatigue in hospitals.
Conclusion: Preventing Alarm Fatigue
To prevent alarm fatigue, it is essential for healthcare teams to prioritize and customize alarms. Prioritizing alarms means setting them to the right levels and ensuring that only important events are receiving an alarm. Customizing alarms allows hospitals to set specific thresholds according to their individual needs or preferences. Additionally, hospitals should aim to reduce the total number of alarms they set off by grouping similar notifications together, disabling those that are unnecessary, or replacing them with other communication methods when appropriate.
Furthermore, hospitals should ensure their clinical staff receives comprehensive training on how to respond appropriately and effectively when a critical alarm occurs. It is also important for healthcare teams to be aware of any existing regulations and standards related to alarm management in order to adhere strictly to them. Finally, hospitals should adopt technologies such as artificial intelligence (AI) which can help detect alarm fatigue before it becomes a problem in order for early intervention strategies can be put in place by clinicians.
Read Also….wellhealthorganic-comhealth-hazards-of-prolonged-sitting